VHA Home HealthCare’s Activation Project is Bringing New Life to Dementia Care
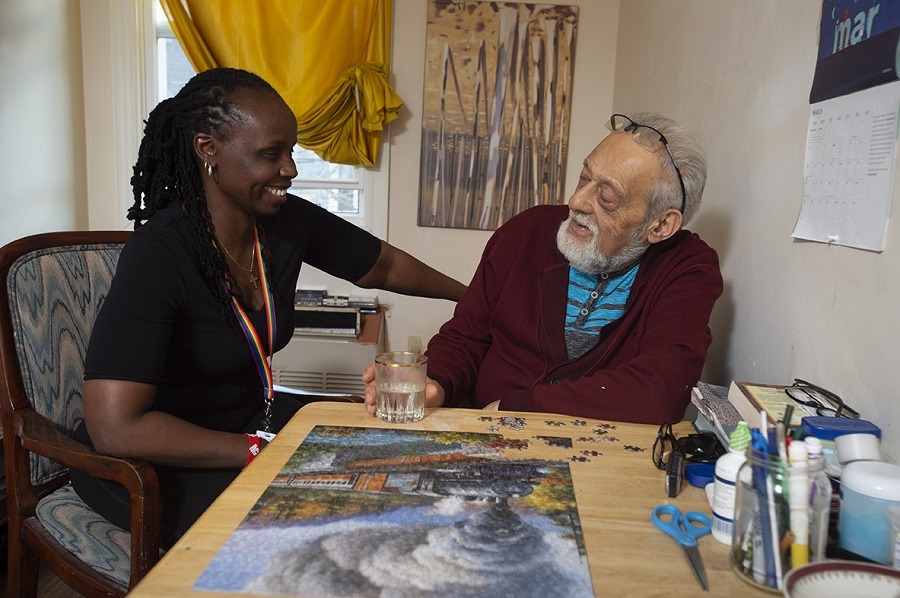
People may not remember exactly what you did, or what you said, but they will always remember how you made them feel – Maya Angelou
Traditional dementia care has long been criticized for being impersonal, unstimulating and too task-focused. Brandi D’Souza, a physiotherapist at VHA Home HealthCare, along with her colleagues Wilfred Leung and Motria Sabat on the Activation Therapy Sub-Committee, have been rethinking the way Personal Support Workers (PSWs) care for dementia patients.
VHA’s efforts are part of a growing movement helping people with dementia live better, more colourful lives. “This model of person-centred care encourages providers to emotionally connect with dementia patients—listen to them, get to know them, trigger positive memories—while meeting their physical needs,” says D’Souza. “This can mean revisiting funny stories from bath time with their kids, smelling spices in the kitchen to see what memories they evoke, or uncovering a hobby that brings them joy,” she explains.
“When we started this project, we realized that many PSWs were already doing a lot of this work. They were either taking the initiative themselves or through cues from supervisors, but they were actively looking for more direction and ideas to make it a part of their care delivery,” notes D’Souza.
This is where the sub-committee’s efforts have been focused. A team of VHA occupational therapists, physiotherapists, PSWs and Client Care Partners developed toolkits to train PSWs on how to put these ideas into practice. The toolkits “are really about emphasising relationships over routine, offering strategies to combat barriers to success and addressing more than just the clinical needs of a dementia patient,” says D’Souza. They include specific ideas for activities, while offering tips for managing difficult behaviours that can make it hard to engage or connect with a client. Activity ideas range from arts and crafts to puzzles to bedside engagement for bedridden patients, and often only require supplies PSWs can find around a client’s home.
Research shows that older adults with dementia who receive this type of care have a better quality of life, experience less of a decline in physical, cognitive and social abilities, and their stress levels go down. “Staff are also more engaged, experience decreased burnout and feel more fulfilled,” Brandi explains.
After many years of experience as a long-term care nurse, VHA Client Partner Elizabeth Hall is also thrilled to be a part this project. While Hall sees this type of care as “excellent and life changing,” she does weigh in on some of the challenges. “When you are moving away from more task-driven care, there needs to be the support and resources in place to allow for these changes,” clarifies Hall. “This means more time allocated with clients, further flexibility in care routines and support from management.” Luckily, VHA is up for the challenge.
In the coming stages, “our organization will continue to look to the community for opportunities to collaborate, evaluate feedback from care providers and clients and further adapt the toolkits to make them as valuable a resource as possible,” says D’Souza.
